Alexandre Gonçalves de SousaI; Maria Zenaide Soares FichinoII; Gilmara Silveira da SilvaIII; Flávia Cortez Colosimo BastosIV; Raquel Ferrari PiottoV
DOI: 10.5935/1678-9741.20140062
ABSTRACT
INTRODUCTION: The knowledge of the prevalence of risk facors and comorbidities, as well as the evolution and complications in patients undergoing coronary artery bypass graft allows comparison between institutions and evidence of changes in the profile of patients and postoperative evolution over time.
OBJECTIVE: To profile (risk factors and comorbidities) and clinical outcome (complications) in patients undergoing coronary artery bypass graft in a national institution of great surgical volume.
METHODS: A retrospective cohort study of patients undergoing coronary artery bypass graft in the hospital Beneficência Portuguesa de São Paulo, from July 2009 to July 2010.
RESULTS: We included 3,010 patients, mean age of 62.2 years and 69.9% male. 83.8% of patients were hypertensive, 36.6% diabetic, 44.5% had dyslipidemia, 15.3% were smokers, 65.7% were overweight/obese, 29.3% had a family history of coronary heart disease. The expected mortality calculated by logistic EuroSCORE was 2.7%. The isolated CABG occurred in 89.3% and 11.9% surgery was performed without cardiopulmonary bypass. The most common complication was cardiac arrhythmia (18.7%), especially acute atrial fibrillation (14.3%). Pneumonia occurred in 6.2% of patients, acute renal failure in 4.4%, mediastinites in 2.1%, stroke in 1.8% and AMI in 1.2%. The in-hospital mortality was 5.4% and in isolated coronary artery bypass graft was 3.5%. The average hospital stay was 11 days with a median of eight days (3-244 days).
CONCLUSION: The profile of patients undergoing coronary artery bypass graft surgery in this study is similar to other published studies.
RESUMO
INTRODUÇÃO: O conhecimento da prevalência dos fatores de risco e comorbidades, bem como a evolução com complicações nos pacientes submetidos à cirurgia de revascularização miocárdica, permite a comparação entre instituições e a comprovação de modificações no perfil de pacientes e na evolução pós-operatória ao longo do tempo.
OBJETIVO: Conhecer o perfil (fatores de risco e comorbidades) e a evolução clínica (complicações) nos pacientes submetidos à cirurgia de revascularização miocárdica em uma instituição nacional de grande volume cirúrgico.
MÉTODOS: Estudo de coorte retrospectivo de pacientes submetidos ao procedimento de cirurgia de revascularização miocárdica no Hospital Beneficência Portuguesa de São Paulo, no período de julho de 2009 a julho de 2010.
RESULTADOS: Foram incluídos 3010 pacientes, com idade média de 62,2 anos e 69,9% do sexo masculino. 82,8% dos pacientes eram hipertensos, 36,6% diabéticos, 44,5% dislipidêmicos, 15,3% tabagistas, 65,7% com sobrepeso/obesidade e 29,3% tinham antecedentes familiares de doença coronária. A mortalidade média esperada calculada pelo EuroSCORE logístico foi de 2,7%. A cirurgia de revascularização miocárdica isolada ocorreu em 89,3% e em 11,9% foi realizada cirurgia sem circulação extracorpórea. A complicação mais comum foi arritmia cardíaca (18,7%), especialmente a fibrilação atrial aguda (14,3%). Pneumonia ocorreu em 6,2% dos pacientes, lesão renal aguda em 4,4%, mediastinite em 2,1%, acidente vascular encefálico em 1,8% e infarto agudo do miocárdio em 1,2%. A mortalidade intra-hospitalar foi de 5,4% e na cirurgia de revascularização miocárdica isolada foi de 3,5%. O tempo de permanência hospitalar médio foi de 11 dias, com mediana de oito dias (3 - 244 dias).
CONCLUSÃO: O perfil dos pacientes submetidos à cirurgia de revascularização miocárdica neste estudo assemelha-se ao de outros estudos publicados.
CABG: Coronary artery bypass graft
LVEF: Ventricle ejection fraction
INTRODUCTION
The likelihood of patients undergoing coronary artery bypass graft (CABG) surgery with a short hospitalization period and no complications depends on the experience of the surgical team, intensive therapy care, the multidisciplinary team involved, and the postoperative follow-up period[1-3].
The success of this procedure is also dependent on the patient's characteristics. In addition to the progress observed in the surgical procedure itself, the population undergoing CABG surgery has also been changing, and this may influence the outcomes. Currently, this population is mucholder, with a higher number of risk factors and associated comorbidities than the population undergoing CABG in the past[4-6]; moreover, increased use of medication drugs modifies the disease's natural course, such as statins[7], as do a high number of previous percutaneous procedures. In Brazil, the number of angioplasties, with or without stenting, increased from 27.5 per 100 thousand inhabitants in 2002 to 39 per 100 thousand inhabitants in 2010[8].
Several national studies have assessed the epidemiology of patients who underwent CABG[9-13]. However, most of those studies focused on specific outcomes or have a long data collection period, with a mean duration of 4-5 years, during which time changes in the profile of the patients may occur, consequently making these studies weak references[6]. Therefore, studies with large samples and short data collection periods are very important in order to assess the demographic profile of patients undergoing CABG in the present.
The aim of this study was to determine the current profile (prevalence of risk factors) and clinical progress of patients undergoing CABG surgery at the Hospital Beneficência Portuguesa in São Paulo.
METHODS
This was a retrospective cohort study; information on patients aged >18 years undergoing the CABG procedure at the Hospital Beneficência Portuguesa in São Paulo, between July 2009 and July 2010, was collected from an electronic database. This database contains data about 3010 patients who underwent CABG, accounting for the data regarding 69.6% of all surgeries performed at the institution over that period. The percentage of patients's loss includedin the database was random, without preference for day, time, period, team, surgeon, or patient condition. The data collection form consisted of 243 variables with data from the preoperative, intraoperative, and postoperative periods (until hospital discharge or death).
The CABG procedure with extracorporeal circulation (ECC) was performed with the patient under general anesthesia and orotracheal intubation in the supine horizontal position, with median transternal longitudinal thoracotomy followed by graft removal (internal thoracic artery, saphenous vein, radial artery, etc.) and inverted-T pericardiotomy. After the bags for ECC were prepared, the patient was given full-dose heparin (3 mg/kg), with arterial cannulation of the ascending aorta, cavoatrial cannulation, insertion of a 14-G catheter in the ascending aorta to connect the aspiration pathways and to infuse a cardioplegic solution, clamping of the ascending aorta, and preparation of the distal and proximal anastomoses, in this sequence.
After this procedure, the ECC system was removed and fluid replacement and protamine infusion (1:1) were performed, along with hemostasis monitoring, draining of the chest cavity and mediastinum, fixing of a pacemaker lead, sternal suturing, and usual closing. In the procedure without ECC, the patient received general anesthesia with orotracheal intubation in the supine horizontal position. Median transsternal longitudinal thoracotomy was performed followed by graft removal (internal thoracic artery, saphenous vein, radial artery, etc.), inverted-T pericardiotomy, heparin administration (1.5 to 3 mg/kg), and preparation of the distal and proximal anastomoses, in this sequence, with the help of a coronary artery stabilizer. After the procedure, the patient was given a protamine infusion (1:1), and hemostasis monitoring and draining of the chest cavity and mediastinum were performed, along with fixing of a pacemaker lead, sternal suturing, and usual closing.
Postoperative complications were defined as:
• Perioperative myocardial infarction: prolonged pain for more than 20 minutes/typical pain not improved with nitrates,and/or seriated electrocardiograms (at least 2) showing new changes to the ST/T segment or new Q waves of at least 0.03 sec or more than a third of the QRS (in at least 2 contiguous leads) plus elevation of cardiac enzyme (creatine kinase-MB or troponin 5 times higher than the normal upper limit) and/or a new hypokinetic area found on echocardiography.
• Stroke: motor deficit persistent for more than 72 hours or coma >24 hours.
• Acute kidney injury: serum creatinine level higher than 2.0 mg/dL or 2 times higher than that in the preoperative period, or the need for dialysis (any method).
• Mediastinitis: deep infection involving the muscles, bones, and/or the mediastinum, with the following conditions: (1) open wound with tissue excision, (2) positive culture results, and (3) treatment with antibiotics.
• Pneumonia: diagnosed on the basis of positive sputum, blood, or pleural fluid culture results; empyema; or radiography showing new infiltrates.
• Arrhythmia: any arrhythmia (atrial fibrillation, atrial flutter, paroxysmal supraventricular tachycardia, brad arrhythmia, or other) requiring intervention.
The study was approved by the Ethics Committee of the Hospital Beneficência Portuguesa in São Paulo under opinion number 663-10.
Statistical considerations
The variables were descriptively analyzed. Regarding the quantitative variables, the analysis was performed by determining the minimum and maximum values and/or the mean, standard deviation, and median values. Regarding the qualitative variables, absolute and relative frequencies were determined.
RESULTS
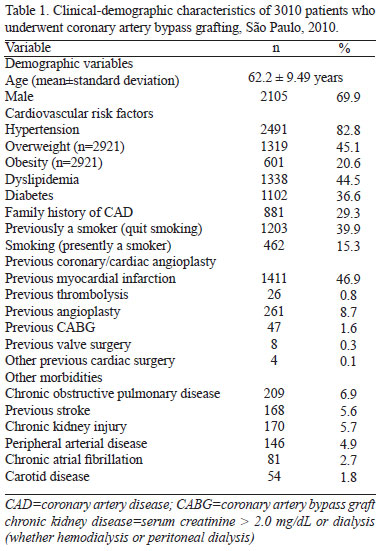
The patients' mean age was 62.2 years, with the proportion of men being 69.9%; 15.3% of the patients were smokers, 82.8%, hypertensive, and 36.6%, diabetic. Regarding the financial aspect, 92.2% of the surgeries were funded by the NHS, 7.0% by private health insurance, and 0.8% by personal resources. The patients' clinical-demographic characteristics are shown in Table 1.
Of the 3010 patients included in this study, 64.6% (1947) had the result of their coronary angiography (catheterization) stated on their patient records. Coronary obstructions larger than 50% were considered serious when located in the left coronary trunk and larger than 70% in all other blood vessels. Similarly, only 44.2% (1331) of the patients had the left ventricle ejection fraction (LVEF) mentioned on their records. In this sample, the method used for estimation of the LVEF was: echocardiography for 1288 patients (96.8%), ventriculography for 30 (2.3%), myocardial scintigraphy for 9 patients (0.7%), and nuclear magnetic resonance imaging for 4 patients (0.3%) (Table 2).

The preoperative risk score (logistic EuroSCORE) was individually calculated for all patients, with the mean score being 2.7 (±3.09) for the group, ranging from 0.88% to 76.6%. The median score was 1.81% (Table 2).
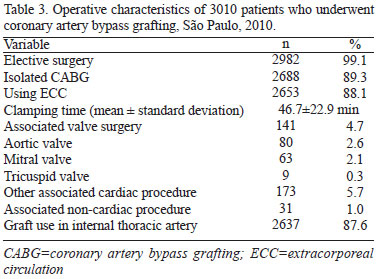
Table 3 shows the characteristics of the surgical procedure.
The frequency of the main postoperative complications is described in Table 4.

The length of the hospital stay was 11 days, with a median of 8 days (range, 3-244 days). Intra-hospital mortality occurred in 162 patients (5.4%). With regard to isolated CABG, the intra-hospital mortality was 3.5%. Intraoperative death occurred in 7 patients (0.2%).
DISCUSSION
The continuous assessment of CABG surgery outcomes using records and large databases is a reality in several countries. The oldest coronary surgery database dates back to 1971 and the most widely publicized one is the United States Society of Thoracic Surgeons' database - STS National Database, which has been collecting data since 1989 and involves more than 800 sites across the country contributing every year with information on approximately 270,000 patients undergoing coronary surgery[14].
In Brazil, although CABG surgeries have been performed for almost half a century, they have not been recorded on a large scale. This study, although not representative of the national situation, presents the immediate reality of an institution with high representativeness at the national level and involving several independent teams.
The results of this study show that men account for the majority of the operated patients (69.9%), in line with other studies that show a proportion of men ranging from 60.0%[15] to 70.0%[16]. Regarding age, an increase in the number of patients belonging to more advanced age groups was observed as opposed to in a study performed at the beginning of the previous decade[17]. This is probably the result of an increasingly aging population and the increased safety in performing the surgery on elderly patients, thereby leading to good results in this population.
The prevalence of cardiovascular risk factors was high, with the most frequent finding being hypertension (82.8%). A high prevalence of hypertension is usually found in studies with this type of population, reaching levels up to 90.7%[17]. Diabetes and obesity showed prevalence rates similar to those reported in the previously mentioned study, whereas the presence of dyslipidemia was relatively lower. It is noteworthy that there is a lower prevalence of smoking in our results than in the results of the other study, with data collected between 2001 and 2002, where the reported rate reaches 63%[18]. This may be the result of numerous awareness and anti-smoking campaigns that took place over the last years. However, the current smoking rate (smoking in the previous 4 weeks) was 15.3% in our study.
The number of patients with previous percutaneous coronary angioplasty has been growing over the last years, high-lighting the increased indication for this procedure[8]. In our series, 8.7% of the patients had a history of percutaneous coronary angioplasty. A study comparing the profile of patients operated in 2 different time periods (early 1990s versus early 2000s) reported a history of coronary angioplasty in 6.5% of patients in the first period and 11% in the second period. Moreover, patient-reported previous stent use in the first moment was none in the first period and 5.8% in the second moment[18]. Regarding the 1099 patients who underwent CABG surgery at the Instituto do Coração (Heart Institute) in São Paulo between May 2007 and June 2009, 14.6%had undergone previous coronary angioplasty[19]. Coronary angiography showed that 77.3% of the patients had severe obstructive lesions in 2 or 3 arteries, a proportion that was practically identical to that reported in a recent study conducted in southern Brazil[20]. Severe left coronary trunk lesions, however, were found in our series at a lower percentage (10.5%) than that reported in other national studies, i.e. 18%[15], 19.2[19] and 21.6%[20].
With regard to surgery, internal thoracic artery use was seen in 87.6% of cases, and this mirrors the concern of the surgery teams for ensuring the implantation of superior grafts whose superiority has been well supported in studies and considered as a quality indicator in CABG surgery.
Regarding ECC use, only 11.9% of the surgeries were performed without ECC support. However, this percentage varied greatly between teams, ranging between 0% and 89.1% for different teams. Data from other national services show that 18.6% of the surgeries were performed without ECC in the southern region[16] and 39.5% of isolated bypass grafting surgeries were performed at the Instituto do Coração, located in the city of São Paulo, from 2000 to 2007[21].
The mean length of hospital stay in this study (11 days) shows a progressive decrease from the length of hospital stay in previous studies. Between 1996 and 1998, the mean was 14.5 days[22] and between 2005 and 2007, 12 days[11].
Comparison of the frequency of postoperative complications between this study and other national data was impossible because of the lack of studies including all the complications. Several studies address this subject by focusing on a specific complication and not on all other complications.
In order to stratify the operative mortality risk, the European Cardiac Surgery Risk Assessment Score (EuroSCORE) was used, a model that was initially validated in 128 sites across Europe[23]. This tool was easy to use and accessible over the Internet, and showed good accuracy in non-European populations as well. In Brazil, although some authors have demonstrated good applicability of the EuroSCORE[24-26], some health services have developed scoring models of their own, better suited to their population[27].
In this study, the isolated CABG mortality was 3.5%. A broad survey using the DATASUS database encompassing 175 hospitals of the NHS showed a mean hospital mortality of 6.22%. Among the hospitals with high volume of surgeries (>100 CABG/year), the mean mortality was 5.77%, ranging between 1.9% and 19%[11].
Advantages and limitations of the study
This study showed the profile of the population who recently underwent CABG surgery at an institution with high volume of surgeries. Several previous publications have assessed the profile of patients undergoing CABG surgery. However, such studies were mostly retrospective, with a long data collection period to obtain a significant sample. This type of data collection may lead to accumulation of several biases arising from changes in the profile of patients over the data collection period as well as from changes in the functioning of the health service itself. In this study, a significant sample was obtained in only 1 year of data collection, thereby minimizing the mentioned effects. The expressive volume of data and the abundance of variables contributed towards the undertaking of several scientific studies in future as well as improvements in the procedure. The variables representing coronary surgery quality led to the setup of an indicator-based quality improvement procedure at the institution, with all the involved surgical team members taking part of it.
The main limitation of this study was the fact that the database used was that of a single institution (single-center), although comprising 14 different surgical teams, with independent procedures. In spite of the broad experience and the high volume of procedures, it cannot be stated that the results are representative of the national scenario, especially of institutions with low volume of surgery. Another limitation was the fact that the data were collected from patient medical records, the quality and completeness of which is dependent on the note-taking skills of the health care team.
CONCLUSION
The clinical-demographic profile of a typical patient undergoing CABG surgery at the Hospital Beneficência Portuguesa in São Paulo is similar to that identified in other studies and mirrors the changes caused by demographic changes and the availability of other therapeutic options.
REFERENCES
1. Lima RC, Kubrusly LF, eds. Diretrizes da cirurgia de revascularização miocárdica, valvopatia e doenças da aorta. Arq Bras Cardiol. 2004;82(supl V):1-20.
2. Guidelines and indications for coronary artery bypass graft surgery: a report of the American College of Cardiology/American Heart Association Task Force on Assessment of Diagnostic and Therapeutic Cardiovascular Procedures (Subcommittee on Coronary Artery Bypass Graft Surgery). J Am Coll Cardiol. 1991;17(3):543-89. [MedLine]
3. Eagle KA, Guyton RA, Davidoff R, Edwards FH, Ewy GA, Gardner TJ, et al.; American College of Cardiology; American Heart Association Task Force on Practice Guidelines; American Society for Thoracic Surgery and the Society of Thoracic Surgeons. ACC/AHA 2004 guideline update for coronary artery bypass graft surgery: summary article: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee to Update the 1999 Guidelines on Coronary Artery Bypass Graft Surgery). Circulation. 2004;110(9):1168-76. [MedLine]
4. Dinh DT, Lee GA, Billah B, Smith JA, Shardey GC, Reid CM. Trends in coronary artery bypass graft surgery in Victoria, 2001-2006: findings from the Australasian Society of Cardiac and Thoracic Surgeons database project. Med J Aust. 2008;188(4):214-7. [MedLine]
5. Clark RE, Edwards FH, Schwartz M. Profile of preoperative characteristics of patients having CABG over the past decade. Ann Thorac Surg. 1994;58(6):1863-5. [MedLine]
6. Ferguson TB Jr, Hammill BG, Peterson ED, DeLong ER, Grover FL; STS National Database Committee. A decade of change--risk profiles and outcomes for isolated coronary artery bypass grafting procedures, 1990-1999: a report from the STS National Database Committee and the Duke Clinical Research Institute. Society of Thoracic Surgeons. Ann Thorac Surg. 2002;73(2):480-9.
7. Walley T, Folino-Gallo P, Schwabe U, van Ganse E; EuroMedStat group. Variations and increase in use of statins across Europe: data from administrative databases. BMJ. 2004;328(7436):385-6. [MedLine]
8. Viacava F, Porto S, Laguardia J, Moreira RS, Ugá MAD. Diferenças regionais no acesso a cirurgia cardiovascular no Brasil, 2002-2010. Ciênc Saúde Colet. 2012;17(11):2963-9.
9. Bianco ACM, Timerman A, Paes AT, Gun C, Ramos RF, Freire RBP, et al. Análise prospectiva de risco em pacientes submetidos à cirurgia de revascularização miocárdica. Arq Bras Cardiol. 2005;85(4):254-61. [MedLine]
10. Oliveira SF, Jatene AD, Solimene MC, Oliveira SA, Meneguetti C, Jatene FB, et al. Cirurgia de revascularização do miocárdio em pacientes com cardiomiopatia isquêmica e disfunção ventricular acentuada: resultados imediatos e de longo prazo. Rev Bras Cir Cardiovasc. 1997;12(1):1-9. View article
11. Piegas LS, Bittar OJNV, Haddad N. Cirurgia de revascularização miocárdica: resultados do Sistema Único de Saúde. Arq Bras Cardiol. 2009;93(5):555-60. [MedLine]
12. Mesquita ET, Ribeiro A, Araujo MP, Campos LAM, Fernandes MA, Colafranceschi AS, et al. Indicadores de qualidade assistencial na cirurgia de revascularização miocárdica isolada em centro cardiológico terciário. Arq Bras Cardiol. 2008;90(5):350-4.
13. Amato VL, Timerman A, Paes AT, Baltar VT, Farsky P, Farran JA, et al. Resultados imediatos da cirurgia de revascularização miocárdica: comparação entre homens e mulheres. Arq Bras Cardiol. 2004;83(no.spe):14-20.
14. Shahian DM, Edwards FH, Ferraris VA, Haan CK, Rich JB, Normand ST, et al.;; Society of Thoracic Surgeons Quality Measurement Task Force. Quality measurement in adult cardiac surgery- conceptual framework and measure selection. Ann Thorac Surg. 2007;83(4 Suppl):S3-12. [MedLine]
15. Campagnucci VP, Silva AMRP, Pereira WL, Chamliam EG, Gandra SMA, Rivetti LA. EuroSCORE e os pacientes submetidos a revascularização do miocárdio na Santa Casa de São Paulo. Rev Bras Cir Cardiovasc. 2008;23(2):262-7. [MedLine] View article
16. Oliveira EL, Westphal GA, Mastroeni MF. Características clínico-demográficas de pacientes submetidos à cirurgia de revascularização do miocárdio e sua relação com a mortalidade. Rev Bras Cir Cardiovasc. 2012;27(1):52-60. [MedLine] View article
17. Oliveira TML, Oliveira GMM, Klein CH, Souza e Silva NA, Godoy PH. Letalidade e complicações da cirurgia de revascularização miocárdica no Rio de Janeiro, de 1999 a 2003. Arq Bras Cardiol. 2010;95(3):303-12. [MedLine]
18. Feier FH, Sant'anna RT, Garcia E, De Bacco FW, Pereira E, Santos MF, et al. Modificações no perfil do paciente submetido à operação de revascularização do miocárdio. Rev Bras Cir Cardiovasc. 2005;20(3):317-22. View article
19. Lisboa LAF, Mejia OAV, Dallan LAO, Moreira LFP, Puig LB, Jatene FB, et al. Intervenção Coronariana Percutânea prévia como fator de risco para Revascularização Miocárdica. Arq Bras Cardiol. 2012;99(1):586-95. [MedLine]
20. Tonial R, Moreira DM. Perfil clínico-epidemiológico dos pacientes submetidos à cirurgia de revascularização do miocárdio no instituto de cardiologia de Santa Catarina, São José- SC. ACM Arq Catarin Med. 2011;40(4):42-6.
21. Lisboa LAF, Moreira LFP, Mejia OAV, Dallan LAO, Pomerantzeff PMA, Costa R, et al. Evolução da cirurgia cardiovascular no instituto do coração: análise de 71.305 operações. Arq Bras Cardiol. 2010;94(2):174-81.
22. Noronha JC, Martins M, Travassos C, Campos MR, Mais P, Panezzuti R. Aplicação da mortalidade hospitalar após a realização de cirurgia de revascularização do miocárdio para monitoramento do cuidado hospitalar. Cad Saúde Pública. 2004;20(Suppl 2):S322-30.
23. Roques F, Nashef SA, Michel P, Gauducheau E, de Vincentiis C, Baudet E, et al. Risk factors and outcome in European cardiac surgery: analysis of the EuroSCORE multinational database of 19030 patients. Eur J Cardiothorac Surg. 1999;15(6):816-22.
24. Moraes Neto F, Duarte C, Cardoso E, Tenório E, Pereira V, Lampreia D, et al. Avaliação do EuroSCORE como preditor de mortalidade em cirurgia de revascularização miocárdica no Instituto do Coração de Pernambuco. Rev Bras Cir Cardiovasc. 2006;21(1):29-34. View article
25. Mejia OAV, Lisboa LAF, Dallan LAO, Pomerantzeff PMA, Moreira LFP, Jatene FB, et al. Validação do 2000 Bernstein-Parsonnet e EuroSCORE no Instituto do Coração - USP. Rev Bras Cir Cardiovasc. 2012;27(2):187-94. [MedLine] View article
26. Sá MPBO, Soares EF, Santos CA, Figueredo OJ, Lima ROA, Escobar RR, et al. EuroSCORE e mortalidade em cirurgia de revascularização miocárdica no Pronto Socorro Cardiológico de Pernambuco. Rev Bras Cir Cardiovasc. 2010;25(4):474-82. [MedLine] View article
27. Gomes RV, Tura B, Mendonça Filho HTF, Campos LAA, Rouge A, Nogueira PMM, et al. RIOEscore: escore preditivo de mortalidade para pacientes submetidos à cirurgia cardíaca baseado em variáveis de pré, per e primeiro dia de pós-operatório. Rev SOCERJ. 2005;18(6):516-26.
No financial support.
Authors' roles & responsibilities
AGS: Database creation, analysis, and manuscript review
MZSF: Database creation and manuscript review
GSS: Database creation and manuscript review
FCCB: Database creation and manuscript review
RFP: Database creation and manuscript review
Article receive on Friday, June 21, 2013
 All scientific articles published at www.bjcvs.org are licensed under a Creative Commons license
All scientific articles published at www.bjcvs.org are licensed under a Creative Commons license