CLINICAL DATA
A one-year-old female white child from Santa Catarina, Brazil, presented with a cardiac murmur during her first month of life. However, no clinical signs were evidenced until she was three months old when she started suffering from cyanosis and hypotonia under effort and a reduction of stature gain. She presented in a good general state, (hydrated and ruddy complexion) but with slight dyspnea and cyanotic ++/4 and the peripheral saturation of O2 at 60%. Ictus cordis presented without alterations with a regular rhythm of two normal sounds and systolic murmur of intense ejection at left sternal border. The pulmonary auscultation was symmetrical, without adventitious sounds. The abdomen presented without alterations. The extremities had symmetrical pulses and good perfusion.
ELECTROCARDIOGRAM
Sinusal rhythm with a frequency of 150 beats per minute was seen. The QRS axis was +120º with right deviation. The right atrium and ventricle were overloaded.
RADIOGRAM
The cardiothoracic index was 0.65. The mean arch was excavated with increase of the right chambers. Pulmonary fields suffered reduced peripheral perfusion.
ECHOCARDIOGRAM
Situs solitus was evidenced at levocardia. The venoatrial connection was abnormal with double inflow tracts at the atrioventricular function from a single right-type ventricle and single atrioventricular valve. There was an ostium primum-type interatrial septum defect, significant infundibular valvar stenosis with a gradient of 77 mmHg and the presence of a patent left superior vena cava.
DIAGNOSIS
A coronary cineangiography confirmed the echocardiographic findings demonstrating double outflow tracts from the single right-type ventricle and significant infundibular valvar pulmonary stenosis. The patent left superior vena cava drained to the coronary sinus. The pressure gradient between the systemic ventricle and the pulmonary branch was 70 mmHg and the mean pulmonary pressure was 12 mmHg.
DIFFERENTIAL DIAGNOSIS
Considering the clinical symptoms, the state is characteristic of congenital heart disease with pulmonary hypoflow, thus, Fallot's tetralogy, pulmonary atresia with interventricular communication, tricuspid atresia and complex heart diseases with single ventricular physiology, should all be considered.
SURGICAL TREATMENT
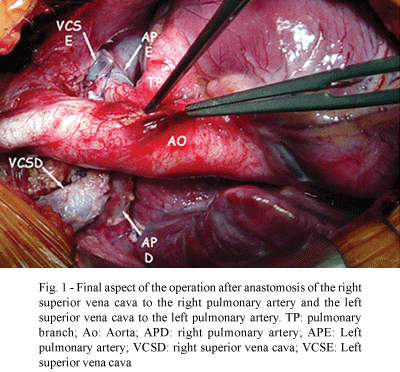
The bicaval bidirectional Glenn operation was possible without the necessity of cardiopulmonary bypass or derivation of the innominate vein to the right atrium or pulmonary branch. Median transsternal thoracotomy was performed and the right superior vena cava was carefully disconnected from the right atrium and anastomosed end-to-side to the right pulmonary artery. Similarly, the left superior vena cava was anastomosed to the left pulmonary artery. The pulmonary branch was submitted to bandaging with the aim of allowing anterograde flow and developing the pulmonary branches. The pressure in the pulmonary branches was measured during the operation, after the anastomosis of the vena cavas and although the anterograde flow was 15 mmHg the patient evolved well in the immediate postoperative period and was discharged from hospital on the eighth postoperative day taking acetylsalicylic acid. The patient should be followed up in the out patients clinic and the Fontan operation should be performed at two years of age.
 All scientific articles published at www.bjcvs.org are licensed under a Creative Commons license
All scientific articles published at www.bjcvs.org are licensed under a Creative Commons license