Murilo Bertazzo PeresI; Ulisses Alexandre CrotiII; Moacir Fernandes de GodoyII; Carlos Henrique De MarchiII; Sírio Hassem SobrinhoII; Lilian BeaniII; Airton Camacho MoscardiniII; Domingo M BraileII
DOI: 10.5935/1678-9741.20140036
ABSTRACT
OBJECTIVE: To evaluate the height and weight development of children with congenital heart disease undergoing surgery with the goal of determining when they reach the threshold of normal development and whether there are differences between patients with developmental pattern below the level of normality preoperatively (z-score<-2 for the analyzed parameter) in comparison to the total group of cardiac patients.
METHODS: We prospectively followed up 27 children undergoing operation into five time periods: preoperatively and at four subsequent outpatient appointments: 1st month, 3rd month, 6th month and 12th month after hospital discharge. The anthropometric parameters used were median z-score (MZ), weight (WAZ), height (HAZ), subscapular skinfold (SSFAZ), upper arm circumference (UAC) and triceps skinfold (TSFAZ). The evolution assessment of the parameters was performed by analysis of variance and comparison with the general normal population from unpaired t test, both in the total group of cardiac patients, and in subgroups with preoperative parameters below the normal level (Zm<-2 ).
RESULTS: In the total group there was no significant evolution of MZ of all parameters. WAZ was statistically lower than the normal population until the 1st month of follow-up (P=0.028); HAZ only preoperatively (P=0.044), SSFAZ in the first month (P=0.015) and at 12th month (P=0.038), UAC and TSFAZ were always statistically equal to the general population. In patients whose development was below the level of normality, there were important variation of WAZ (P=0.002), HAZ (P=0.001) and UAC (P=0.031) after the operation, and the WAZ was lower than the normal population until the 3rd month (P=0.015); HAZ and UAC, until the first month (P=0.024 and P=0.039 respectively), SSFAZ, up to the 12th month (P=0.005), the TSFAZ only preoperatively (P=0.011).
CONCLUSION: The operation promoted the return to normalcy for those with heart disease in general within up to three months, but for the group of patients below normal developmental pattern of the return occurred within 12 months.
RESUMO
OBJETIVO: Avaliar a evolução pôndero-estatural de crianças com cardiopatias congênitas submetidas a tratamento cirúrgico com intuito de determinar quando atingem o limiar de desenvolvimento normal e se há diferenças entre pacientes com padrão de desenvolvimento abaixo do patamar da normalidade no pré-operatório (z-score<-2 para o parâmetro analisado) em relação ao grupo total de cardiopatas.
MÉTODOS: Acompanhamento prospectivamente de 27 crianças submetidas à operação em cinco períodos: pré-operatório e em quatro subsequentes retornos ambulatoriais: 1º mês, 3º mês, 6º mês e 12º mês após a alta hospitalar. Os parâmetros antropométricos usados foram a média do z-score (Zm) do peso (ZmP/I), da altura (ZmA/I), prega cutânea subescapular (ZmPCS/I), perímetro braquial (ZmPB/I) e prega cutânea tricipital (ZmPCT/I). A avaliação da evolução dos parâmetros foi feita pela análise de variância e a comparação com a população geral normal pelo teste t não pareado, tanto no grupo total dos cardiopatas, quanto nos subgrupos com parâmetros pré-operatórios abaixo do patamar da normalidade (Zm<-2).
RESULTADOS: No grupo total não houve evolução significativa dos Zm de todos os parâmetros. O ZmP/I foi estatisticamente menor que da população normal até o 1º mês de seguimento (P=0,028); o ZmA/I, somente no pré operatório (P=0,044); o ZmPCS/I, no o 1º mês (P=0,015) e no 12º mês (P=0,038); o ZmPB/I e o ZmPCT/I sempre foram estatisticamente iguais ao da população geral. Nos pacientes com desenvolvimento abaixo do limiar da normalidade houve variação importante do ZmP/I (P=0,002), do ZmA/I (P=0,001) e do ZmPB/I (P=0,031) após a operação, sendo que o ZmP/I foi menor que da população normal até o 3º mês (P=0,015); o ZmA/I e o ZmPB/I, até o 1º mês (P=0,024 e P=0,039 respectivamente); o ZmPCS/I, até o 12º mês (P=0,005); o ZmPCT/I, somente no pré-operatório (P=0,011).
CONCLUSÃO: A operação promoveu o retorno à normalidade para os cardiopatas em geral dentro de até três meses, porém para o grupo de pacientes abaixo do padrão normal de desenvolvimento o retorno ocorreu em até 12 meses.
IVC: interventricular communication
IAC: interatrial communication
CoA: coarctation of the aorta
SD: Standard Deviation
AVSD: (partial) atrioventricular septal defect
WHO: World Health Organization
PDA: patent ductus arteriosus
SUS: Unified Health System
HAZ: Height/Age Z-score
TSFAZ: triceps skinfold/age Z-score
MZ-score: Median Z-scores
WAZ: Weight/age Z-scores
BPAZ: brachial perimeter/age Z-score
SSFAZ: subscapular skinfold/age Z-score
TSFAZ: triceps skinfold/age TOF cyanotic tetralogy of Fallot
INTRODUCTION
The prevalence of congenital heart disease is approximately 6/1000 live births, the most common severe congenital anomaly and having important implications in mortality in the first year of life[1,2]. In our environment, Guitti estimated a prevalence of 5.4 / 1,000 live births, with interventricular communication (IVC) as the most common injury found[3].
Congenital heart defects usually cause changes in development, mainly in height and weight, which when measured are shown below the normal mean for age[4-8]. These changes are usually multifactorial and may be from both cardiac and extra-cardiac causes[8-10].
The advancement of corrective surgeries had great impact on the improvement of growth and weight gain in these patients[11-14], but it always dependent on factors such as the severity of the initial underdevelopment, the presence or absence of cyanosis, the hemodynamic status, pre-natal causes and fundamentally the type of disease[12-20].
Divergences about how these children can develop after surgery prompted us to evaluate the weight-height evolution in order to determine when they reach the threshold of normal development and whether there are differences between patients with standard development below the level of normality in the preoperative period (z-score <-2 for the parameter analyzed) compared to the total group of cardiac patients.
METHODS
From October 2009 to June 2011, 27 children with congenital heart disease admitted to perform corrective surgery were studied in the Department of Pediatric Cardiovascular Surgery, School of Medicine of São José do Rio Preto, Hospital de Base (FAMERP), São Paulo, Brazil.
The study was approved by the Research Ethics Committee of the Institution (Opinion No. 181/2009 and Protocol 3088/2009).
The mean age was 27.6 months, ranging 3-115 months with a standard deviation of 26.7 months and a median of 20.1 months. Twelve were male (44.4%). The diagnosis in 17 children was acyanogenic disease, seven with interatrial communication (IAC), five with atrial septal defect (ASD), one with partial ventricular septal defect (PVSD), two with patent ductus arteriosus (PDA) and two with coarctation of the aorta (coarctation). The other 10 children had tetralogy of Fallot (TOF).
The study included children whose families accepted the Informed Consent for outpatient follow-up period of at least one year. We excluded premature patients, and patients with genetic syndromes or noncardiac causes of malnutrition.
Weight, height, subscapular skinfold, brachial perimeter and triceps skinfold were measured in the preoperative periods and in four subsequent outpatient care moments: 1st month, 3rd month, 6th, month and 12th month after hospital discharge.
Weight was measured with properly calibrated pediatric scales[21-23]. The measures were determined with the aid of a pediatric digital scale (Filizola®), with a maximum of 15 kg and 5g division.
We also used a caliper of Sanny ® brand precision of tenths of a millimeter, a measuring tape in millimeters and a children's anthropometer to obtain height measurement [21-23].
The subscapular skinfold was determined obliquely to the longitudinal axis of the body, following the guidance of ribs two inches below the inferior angle of the scapula[23].
The brachial perimeter was obtained as the measurement of the circumference at the middle third of the arm[23].
The triceps skinfold was measured on the posterior side of the arm, at the midpoint between the upper lateral edge of the acromion and the inferior border of the olecranon. The measurement was carried out following the longitudinal axis of the member[23].
All children were measured by the same person, with the same instruments and the same environment, in other words, in the Cardiopediatrics Outpatient of Hospital de Base. Each measurement was repeated three times and the mean value found was considered for the study[21-23].
The z-scores were calculated in relation to age, and for weight/age (WAZ), height/age (HAZ), brachial perimeter/age (BPAZ), subscapular skinfold/age (SSFAZ), triceps skinfold/age (TSFAZ), based on the WHO Anthro program of the World Health Organization (WHO)[24,25].
Based on the WHO growth curves, we considered z-scores values -2 or less, for any parameter used, as being below the normal standard of weight and height[24,25] development.
Statistical analysis was performed with the aid of Stats Direct Statistical Software Version 1.9.15. Values ??of continuous variables were expressed as means and standard deviation (SD). We used analysis of variance to perform the comparison of the evolution of the values ??of the mean z-scores (MZ) over this period, for all anthropometric parameters (WAZ, HAZ, BPAZ, SSFAZ, TSFAZ), and Dunnett's post-test analysis in case of detection of statistically significant difference. The unpaired two-tailed Student's t test was performed to compare the values ??of MZ in each follow-up period with the normal general population, which was considered as a z-score of 0 and SD of 2.
These tests were applied specifically in the total group of patients with cardiac disesases and in the subgroups of cardiac patients below the normal development pattern in the preoperative period according to the anthropometric parameter analyzed (in subgroups of patients with z-score below -2 in the preoperative period to the parameter analysed).
It was assumed a 5% alpha error with significance level of P<0.05. The representation has been demonstrated with the aid of Box plot graphs.
RESULTS
All measurements were taken in 27 children in the preoperative period, but there were some flaws during the follow-up, and only 14 of them were evaluated in the 1st month, 16 in the 3rd month, 18 in the 6th month and 16 in the 12th month.
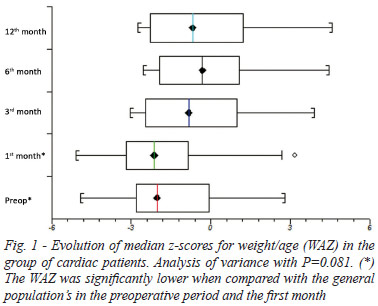
The was no statistical significance in WAZ for the analysis of variance over the study period for the total group of cardiac patients (P=0.081). For the group with the WAZ below the normal pattern of development related to the preoperative analysis of variance demonstrated statistical significance (P=0.002), and the post-test analysis demonstrated statistical difference in WAZ during the preoperative period with WAZ of the 6th month (P=0.011) and 12th month (P=0.006).
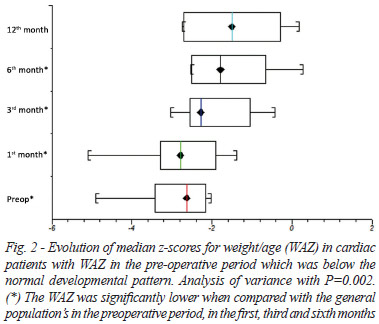
The WAZ of the total group of cardiac patients was significantly lower than the general population's only in the preoperative period (P=0.008) and during the 1st month (P=0.028). The WAZ in the group below the normal pattern of development was lower than the general population's only in the preoperative period (P<0.001) in the 1st month (P=0.001) in the 3rd month (P=0.015), and in the 6th month (P=0.047) of the follow-up period.
Figures 1 and 2 demonstrate the evolution of the WAZ for the total group of cardiac patients and for the group of cardiac patients with WAZ in the preoperative period below normal developmental pattern.
In HAZ there was no statistical significance in the analysis of variance over the study period for the total group of cardiac patients (P=0.182). For children with HAZ in the preoperative period below normal development pattern the analysis of variance demonstrated statistical significance (P=0.001), and the post-test analysis showed statistical difference in HAZ in the preoperative period with HAZ of the 3rd month (P = 0.040), the 6th month (P=0.007) and the 12th month (P<0.001).
The HAZ of the total group of cardiac patients was significantly lower than the general population's only in the preoperative period (P=0.044). The HAZ in the group below the normal pattern of development was lower than the general population's in the preoperative period (P=0.028) in the 1st month (P=0.024) during the follow-up.
Figures 3 and 4 demonstrate the evolution of HAZ for the total group of patients with cardiac complications and for the group of cardiac patients with HAZ in the preoperative period below normal developmental pattern.


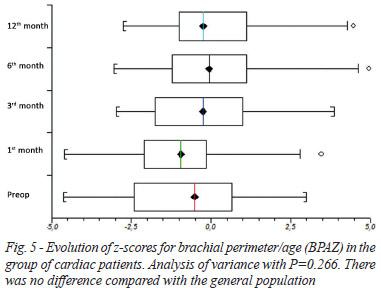
There was no statistical significance for the BPAZ in the analysis of variance for the total group of cardiac patients (P=0.266). For children with BPZ in the preoperative period below normal development pattern, the analysis of variance demonstrated statistical significance (P=0.031), and the post-test analysis demonstrated statistical difference in BPAZ in the preoperative period compared to those from the 6th month (P= 0.045) and 12th month (P= 0.031).
The BPAZ of the total group of cardiac patients was not significantly lower than the general population's in any period. The BPAZ in the group below the normal pattern of development was lower than the general population's only in the preoperative period (P= 0.058) and in the 1st month (P=0.036).
Figures 5 and 6 show the evolution of BPAZ for the total group of patients with cardiac problems and for the group of cardiac patients below the normal pattern of development.

The SSFAZ showed no statistical significance in the analysis of variance for the total group of cardiac patients (P=0.514). For children with SSFAZ in the preoperative period below normal developmental pattern, the analysis of variance also did not show statistical significance (P=0.101).
The SSFAZ of the total group of cardiac patients was significantly lower than the general population's in the preoperative period (P<0.001) in the 1st month (P=0.015) and in the 12th month (P=0.038). The SSFAZ in the group below the normal pattern of development was lower than the general population's in the preoperative period (P<0.001) in the 1st month (P=0.066) the 3rd month (P=0.004) the 6th month (P=0.038) and in the 12th month (P=0.005).
Figures 7 and 8 show the evolution of SSFAZ for the total group of patients with cardiac diseases and for the group with cardiac patients below the normal pattern of development.


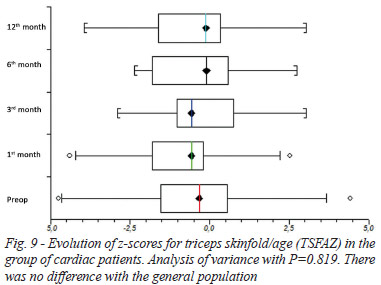
There was no statistical significance in TSFAZ in the analysis of variance for the total group of cardiac patients (P=0.819). For children with TSFAZ in the preoperative period below normal development pattern, the analysis of variance did not show statistical significance (P=0.054).
The TSFAZ of the total group of cardiac patients was not significantly lower than the general population's in the analyzed periods. It was lower in the group below the normal pattern of development than the general population's in the preoperative period (P=0.011), as can be seen in Figures 9 and 10.

DISCUSSION
As already mentioned by several authors, patients with congenital heart disease have a deficit in weight and height development[4-6,8,17]. The low energy intake, hypermetabolism[8,9] and cell hypoxia[9] are factors that decrease the availability of energy and hamper the adoption of a proper diet for these children, contributing to their developmental delay [10,15].
Hemodynamic factors such as cyanosis, hypertension and heart failure are implicated in the worsening of the energy expenditure, leading to a growth disorder[7,14,15,17,20]. The pulmonary hypertension seems to be the most relevant, to increase oxygen consumption by the right ventricle, which can often be hypertrophic or dilated by volume overload [7,15,17,20].
Factors restricting growth potential are also implicated in growth retardation of cardiac patients, such as low birth weight, small for gestational age and associated genetic syndromes [7,11,17].
In the total group of cardiac patients, the present study found no significant variation of MZ for all parameters analyzed during the first 12 months after the operation, which can be evidenced by analysis of variance. This may indicate that these parameters require outpatient treatment longer than a year to demonstrate significant variation in this specific group of patients, and also suggest that the sample was insufficient or small for the proposed study.
In the groups of patients with heart diseases below normal development pattern in the preoperative period, those with z-score below -2, there was significant variation in weight, height and brachial parameter, indicating that corrective surgery was of utmost importance for rapid weight and height recovery.
Weight and height proved to be good parameters for the analysis of evolution in the total group of cardiac patients, with recovery in the 3rd and 1st month respectively, becoming statistically similar to the general population. The same occurred with the group of patients with below normal developmental pattern in the preoperative period for weight and height, with recovery in the 12th and 3rd month. Therefore, the weight and height seem to be the best parameters for routine outpatient follow-up.
The TSFAZ and BPAZ in the total group of cardiac patients were not lower than the general population's for the time periods examined, in other words, they were always within the normal range, showing that these parameters may not be useful in people with heart disease in general as the analysis tool of weight-height development, since they require a serious initial commitment for being altered. In the groups of cardiac patients below normal developmental pattern in the preoperative period for the same parameters, the tricips skinfold was normalized in the 1st month and the brachial perimeter in the 3rd month, showing that these parameters may be useful for the follow-up of severely malnourished children, and especially BPAZ, which showed statistically significant variation and indicated to be a parameter of rapid improvement after corrective cardiac surgery.
The SSFAZ in the total group of cardiac patients showed recovery from the 3rd month of the follow-up period, however, it is probably not a very reliable parameter because the difficulty of its measurement may cause measurement errors, which may explain what happened in the 12th month, with a drop of recovery over the general population. Moreover, in the group with heart disease patients' below normal developmental pattern in the preoperative period for subscapular skinfold, the measure remained below the general population throughout the follow-up, indicating that it is probably a parameter of delayed recovery in malnourished patients and, therefore it is necessary a longer follow-up to analyze the recovery to the normal parameters.
Numerous studies show that after surgery, children with heart disease benefit from the recovery to its normal state of development within one year[11-15], which is in agreement with our findings. Vaidynathan et al.[14] also found similar results to ours, with significant increase in WAZ from the 3rd month of the follow-up period.
However, few studies include the perimeter and skinfolds to assess the development, and Silva VM et al.[4] positively correlated with subscapular skinfold with weight and height percentile values with age, confirming our findings that this anthropometric measurement may be useful in monitoring children with heart disease to assess the degree of malnutrition, despite its technical difficulties. Besides not presenting good energy reserves, heart diseases also provides a low-calorie-and-fat[10] contribution, which favors the involvement of subcutaneous reserves in the measured location.
This study demonstrated that children most severely malnourished in the preoperative period received the most benefits from the operation, increasing their weight and height parameters within the first year, which is consistent with the literature. However, this recovery is slower than in individuals in general, precisely because of the degree of malnutrition in the preoperative period[13-16].
Major limitations of the study
This was a prospective study that required regular monitoring of children and all of them were treated by the Unified Health System (SUS) in a tertiary referral center serving a wide geographic area. Therefore we faced some limiting factors such as economic hardship and distance to attend the follow-up appointments. Thus, the number of patients was not constant in the follow-up months, which was partly offset by appropriate statistical analysis.
The hemodynamic or clinical variables such as pulmonary hypertension or degree of preoperative cyanosis were not considered, which are constantly mentioned in the literature as an aggravating factor in height and weight recovery[7,15,17].
Birth weight was also not assessed, which is known as an aggravating factor in height and weight development[6,7,14], however premature infants were excluded.
CONCLUSION
Children with congenital heart disease undergoing operation return to normal height and weight evolution within 3 months, and those that are below the normal developmental pattern in the preoperative period receive the most benefits, returning to normal evoluiton within 12 months.
REFERENCES
1. Hoffman JIE, Kaplan S. The incidence of congenital heart disease. J Am Coll Cardiol. 2002;39(12):1890-900. [MedLine]
2. Rivera IR, Silva MAM, Fernandes JMG, Thomaz ACP, Soriano CFR, Souza MGB. Cardiopatia congênita no recém-nascido: da solicitação do pediatra à avaliação do cardiologista. Arq Bras Cardiol. 2007;89(1):6-10. [MedLine]
3. Guitti JCS. Aspectos epidemiológicos das cardiopatias congênitas em Londrina, Paraná. Arq Bras Cardiol. 2000;74(5):395-9.
4. Silva VM, Lopes MVO, Araujo TL. Evaluation of the growth percentiles of children with congenital heart disease. Rev. Latinoam Enferm. 2007;15(2):298-303.
5. Tefuarani N, Hawker R, Vince J, Sleigh A, Williams GM. Surgical programme at Royal Alexandra Hospital, Sidney, for Papua New Guinea children with congenital heart disease, 1978-1994. J Paediatr Child Health. 2002;38(2):178-82. [MedLine]
6. Amorim LFP, Pires CAB, Lana AMAL, Campos AS, Aguiar RALP, Tibúrcio JD, et al. Apresentação das cardiopatias congênitas diagnosticadas ao nascimento: análise de 29.770 recém-nascido. J Pediatr. 2008;84(1):83-90.
7. Levy RJ, Rosenthal A, Miettinen OS, Nadas AS. Determinants of growth in patients with ventricular septal defect. Circulation. 1978;57(4):793-7. [MedLine]
8. Menon G, Poskitt EM. Why does congenital heart disease cause failure to thrive? Arch Dis Child. 1985;60(12):1134-9. [MedLine]
9. Weintraub RG, Menahem S. Growth and congenital heart disease. J Paediatr Child Health. 1993;29(2):95-8. [MedLine]
10. Vieira TCL, Trigo M, Alonso RR, Ribeiro RHC, Cardoso MRA, Cardoso ACA, et al. Avaliação do consumo alimentar de crianças de 0 a 24 meses com cardiopatia congênita. Arq Bras Cardiol. 2007;89(4):219-24. [MedLine]
11. Bravo-Valenzuela NJM, Passarelli MLB, Coates MV, Nascimento LFC. Recuperação pôndero-estatural em crianças com síndrome de Down e cardiopatia congênita. Rev Bras Cir Cardiovasc. 2011;26(1):61-8. [MedLine] View article
12. Cheung MM, Davis AM, Wilkinson JL, Weintraub RG. Long term somatic growth after repair of tetralogy of Fallot: evidence for restoration of genetic growth potential. Heart. 2003;89(11):1340-3. [MedLine]
13. Schuurmans FM, Pulles-Heintzberger CF, Gerver WJ, Kester AD, Forget PP. Long-term growth of children with congenital heart disease: a retrospective study. Acta Paediatr. 1998;87(12):1250-5. [MedLine]
14. Vaidynathan B, Nair SB, Sundaram KR, Babu UK, Shivaprakasha K, Rao SG, et al. Malnutrition in children with congenital heart disease (CHD) determinants and short term impact of corrective intervention. Indian Pediatr. 2008;45(7):541-6. [MedLine]
15. Tokel K, Azak E, Ayabakan C, Varan B, Aşlamaci SA, Mercan S. Somatic growth after corrective surgery for congenital heart disease. Turk J Pediatr. 2010;52(1):58-67. [MedLine]
16. Manso PH, Carmona F, Jácomo AD, Bettiol H, Barbieri MA, Carlotti AP. Growth after ventricular septal defect repair: does defect size matter? A 10-year experience. Acta Paediatr. 2010;99(9):1356-60. [MedLine]
17. Varan B, Tokel K, Yilmaz G. Malnutrition and growth failure in cyanotic and acyanotic congenital heart disease with and without pulmonary hypertension. Arch Dis Child. 1999;81(1):49-52. [MedLine]
18. Pinheiro DGM, Pinheiro CHJ, Marinho MJF. Comprometimento do desenvolvimento pondo-estatural em crianças portadoras de cardiopatias congênitas com shunt cianogênico. Rev Bras Promoç Saúde. 2008;21(2):98-102.
19. Huber J, Peres VC, Santos TJ, Beltrão LF, Baumont AC, Cañedo AD, et al. Cardiopatias congênitas em um serviço de referência: evolução clínica e doenças associadas. Arq Bras Cardiol. 2010;94(3):333-8.
20. Leite HP, Carvalho ACC, Fisberg M. O estado nutricional de crianças portadoras de cardiopatia congênita com shunt esquerda-direita: importância da presença de hipertensão pulmonar. Arq Bras Cardiol. 1995;65(5):403-7. [MedLine]
21. Vannucchi H, Unamuno MRL, Marchini JS. Avaliação do estado nutricional. Medicina (Ribeirão Preto). 1996;29(1):5-18.
22. Marcondes E. Pediatria Básica. 9. ed. São Paulo: Sarvier; 2002.
23. Frisancho AR. Anthropometric standards for the assessment of growth and nutritional status. 1. ed. Ann Arbor: University of Michigan Press; 1990.
24. WHO. Multicentre Growth Reference Study Group. WHO Child Growth Standards: Length/height-for-age, weight-for-age, weight-for-length, weight-for-height and body mass index-for-age: Methods and development. Geneva: World Health Organization; 2006.
25. WHO. Multicentre Growth Reference Study Group. WHO Child Growth Standards: Head circumference-for-age, arm circumference-for-age, triceps skinfold-for-age and subscapular skinfold-for-age: Methods and development. Geneva: World Health Organization; 2007.
The study received financial support from the Scientific Initiation Scholarship Program (BIC2009/2010) at the School of Medicine of São José do Rio Preto (FAMERP)
Authors' roles & responsibilities
MBP: Autor principal
UAC: Coautor
MFG: Coautor
CHM: Coautor
SHS: Coautor
LB: Coautor
ACM: Coautor
DMB: Coautor
Article receive on Thursday, June 6, 2013
 All scientific articles published at www.bjcvs.org are licensed under a Creative Commons license
All scientific articles published at www.bjcvs.org are licensed under a Creative Commons license