Karla ReichertI; Helison Rafael Pereira do CarmoI; Fany LimaI; Anali Galluce TorinaI; Karlos Alexandre de Souza VilarinhoII; Pedro Paulo Martins de OliveiraII; Lindemberg Mota Silveira FilhoII; Elaine Soraya Barbosa de Oliveira SeverinoII; Orlando PetrucciIII
DOI: 10.5935/1678-9741.20130085
ANOVA Analysis of variance
ATP Adenosine triphosphate
G/A Glutamate/aspartate cardioplegic solution
HE Hematoxylin and eosin
HTK Histidine-tryptophan cardioplegic solution
INTRODUCTION
Elective cardiac arrest was first performed by global myocardial ischemia with aortic cross-clamping in combination with hypothermia, as reported by Lewis & Taufic [1]. Since then, complex open-heart surgeries with longer aortic cross-clamp periods have been developed. However, the use of longer cross-clamp periods has increased the incidence of ischemia/reperfusion injury. In 1955, Melrose et al. [2] introduced the concept of pharmacologic cardiac arrest, named cardioplegia, which could be obtained by using a solution with a high potassium concentration. Cardioplegic solutions with moderate potassium concentrations were introduced into surgical practice in the mid-1970s and have remained the gold standard for myocardial protection [3,4]. Today, most cardiac surgeries are performed by cardiopulmonary bypass with pharmacologic cardioplegic arrest.
The elevated extracellular potassium level provided by the cardioplegic solution shifts the resting myocyte membrane potential from -85 mV to a range between -65 and -40 mV. This shift inactivates the fast sodium channels, thereby blocking conduction of the myocardial action potential and inducing a "depolarized" arrest. However, an inward non-inactivating sodium "window" current occurs at these higher membrane potentials [5,6]. This condition can lead to intracellular sodium loading and calcium overload of the myocyte, resulting in contracture and cell death [7].
The relative benefits provided by different cardioplegic solutions remain unclear. We idealized a new, potassium-free cardioplegic solution, named LIRM solution, containing: cromakalim, a potassium adenosine triphosphate (ATP)-channel opener that causes hyperpolarization of the cell membrane and coronary artery vasodilation [8]; lidocaine, a sodium-channel blocker that inhibits sodium influx into the myocyte and depolarization of the cell membrane [9]; and 2,3-butanedione, a direct myofilament inhibitor that prevents myocyte contraction by desensitizing the myofilament calcium [10]. In the present study, we tested the myocardial protection afforded by the LIRM solution in terms of the ATP myocardial content and caspase 3 activity, which are important factors for short- and long-term outcomes for heart transplant and conventional open-heart surgeries [4,11-13]. We compared the myocardial protection results among the LIRM, histidine-tryptophan (HTK), and glutamate/aspartate (G/A) cardioplegic solutions after 4 hours of cold storage.
METHODS
Surgical protocol
Wistar male rats (250-350 g) were anesthetized by intraperitoneal injection of sodium thiopental (150 mg/kg). The protocol design in this study was intended to recreate the heart situation after aortic clamp release and right before heart reperfusion. The animals underwent tracheostomy and were mechanically ventilated (Minivent, Harvard Apparatus, Holliston, MA, USA). The chest was opened with a median sternotomy, the right carotid artery was catheterized, and the transverse aortic arch was isolated between the brachiocephalic artery and the left carotid artery. The transverse arch was tied, and cardioplegic solution was injected at an infusion rate of 5 mL/min. The total dose for arresting the heart was recorded. Three different cardioplegic solutions were evaluated.
The heart was excised and kept at 4ºC for 4 hours, simulating the period of arrest for a transplant or a long period of aortic cross-clamp time. At the end of this period, the heart was snap-frozen in liquid nitrogen. A sample tissue of each group was evaluated with hematoxylin and eosin (HE) staining for gross assessment of the cell anatomy.
All procedures were performed in accordance with the "Guide for the Care and Use of Laboratory Animals" published by the US National Institutes of Health (NIH Publication No. 85-23, revised 1996) and the Brazilian Council in Animal Experimentation (COBEA).
Cardioplegic solutions
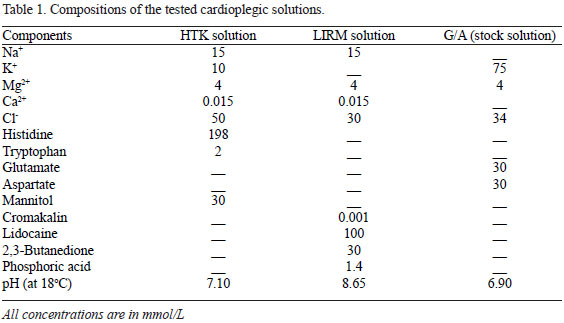
The compositions of the tested cardioplegic solutions are shown in Table 1. The G/A solution (Braile Biomédica, São José do Rio Preto, Brazil) was diluted to 1% before delivery to the heart.
Determination of the myocardial ATP and caspase 3 activity levels
Myocardial tissue was removed from the liquid nitrogen, kept in the same proportion of extraction buffer, and homogenized with 25 mM Tris-HCL, 150 mM NaCl, 1% NP-40, 1% sodium deoxycholate, and 0.1% SDS. The homogenized tissue was centrifugated at 10,000 × g for 40 minutes at 4ºC. The supernatant was used for ATP assessment. Myocardial ATP levels were assessed with the ENLITEN ATP assay system (Promega, Madison, WI, USA) and a Glomax 20/20 (Promega) for bioluminescence quantification, according to the manufacturer's instructions. The ATP level was measured relative to ATP standards provided by the manufacturer. The caspase 3 activity (in relative units of activity) was assessed with the Caspase-Glo 3 Assay (Promega), according to the manufacturer's instructions.
Determination of cytotoxicity
L929 cells (Genetech Inc. South San Francisco, CA, USA) were incubated at 37ºC under an atmosphere of 5% CO2. Cardioplegic solutions were added to the cultured cells at progressive dilutions, and the cells were evaluated 24 hours later. The cell viability was assessed with the MTT (dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide) colorimetric method. Readings were performed at a wavelength of 550 nm [14].
Statistical analysis
All values were expressed as the mean ± standard deviation (SD). Variables were tested for normal distribution. One-way analysis of variance (ANOVA) or Kruskal-Wallis test was applied where appropriate. Differences with a P-value < 0.05 were considered statistically significant. All graphs and statistical analyses were performed with the GraphPad Prism version 6 software package for the Mac OS X (GraphPad Software, La Jolla, CA, USA).
RESULTS
The animals showed comparable weights. Compared to the HTK and G/A solutions, less volume of LIRM solution was needed to achieve cardiac arrest (P=0.008) (Table 2).

Histological findings
The HE plates of the three cardioplegic solutions showed similar findings, with no gross disruption of the cell architecture or edema after 4 hours of cold preservation (Figure 1).
ATP myocardial content and caspase 3 activity levels
The ATP myocardial content after 4 hours of cold storage was higher in the HTK solution group, with no differences between the LIRM and G/A groups (Figure 2A). The caspase 3 activity was higher in the G/A group compared to that of the LIRM and HTK groups, whereas the LIRM group showed higher caspase activity compared to the HTK group (Figure 2B).
Cell viability
None of the solutions showed cytotoxicity after contact with L929 cells for 24 hours (Figure 3).

DISCUSSION
In this study, we evaluated the effect of three different cardioplegic solutions on myocardial ATP content and caspase 3 activity after 4 hours of cold conservation. We also evaluated cell cytotoxicity after 24 hours of exposure to the cardioplegic solutions. The ATP myocardial content was higher in the HTK group compared to the G/A and LIRM groups. The caspase 3 activity was the lowest in the HTK and highest in the G/A group. Peculiarly, the caspase 3 activity showed an intermediate activity with the LIRM solution compared to the two other solutions. None of the solutions demonstrated cytotoxicity in cell culture, a finding that is not often reported in the literature regarding cardioplegic solutions [15,16].
Our findings confirm the effectiveness of HTK solution as an organ preservation solution, as demonstrated by ATP conservation. Another important finding was the lower activity of caspase 3 with HTK solution, which is not often reported [17]. The LIRM solution showed a beneficial effect on caspase 3 activity and a very effective ability to arrest the heart without potassium. The ideal cardioplegic solution, which has yet to be determined, should allow a rapid and effective induction of diastolic arrest, should minimize ischemia/reperfusion injury, and should have no deleterious effects on other organs [18]. The rapid and effective induction of cardiac arrest may minimize myocardial ATP depletion and contribute to the protective effects during the reperfusion period [18-20]. In the present study, the LIRM solution displayed a pronounced capacity to promote cardiac arrest compared to the other two solutions. However, the myocardial ATP content was very similar when the LIRM and G/A solutions were used. Regardless of the cause, the caspase 3 activity of the LIRM solution was lower than that of the G/A solution, which might represent an improvement during the reperfusion period. An analysis of the details of this concept is beyond of the scope of the current study.
The HTK solution effectively reduced the energy requirements, as observed in this and previous studies [21]. However, other reports have shown an inability of HTK solution to reduce endothelial dysfunction after long periods of cold storage [22]. The LIRM solution contains cromakalin, which has beneficial effects on endothelial function and coronary vasodilation. Nevertheless, the beneficial effects of this agent were not tested in the present study design [23].
To induce a pharmacologic arrest, the arresting agents of a cardioplegic solution must interact with some targets involved in excitation-contraction coupling. This effect can be reached by inhibiting the myocardial action potential propagation and/or inhibiting calcium activation of the myofilaments. The LIRM solution has components to induce cardiac arrest by both of these mechanisms. The LIRM solution contains three different agents (cromakalin, 2,3-butanedione, and lidocaine) at very low concentrations to induce cardioplegic arrest without hyperkalemia. All three components were added to the initial formula for sum effect and to avoid any deleterious effects of the higher concentration of one isolated component. The other solutions tested in this report induce cardiac arrest by different mechanisms. The G/A solution induces cardiac arrest by inhibiting the action potential by hyperkalemia, leading to depolarization of the cell membrane. The HTK solution does the same, inhibiting the myofilament action by providing a very low calcium concentration.
Although universally used, the strategy of depolarized arrest with hyperkalemia has distinct disadvantages. In particular, cellular ionic currents are maintained during the ischemia/arrested period, which can lead to adverse effects [18,24]. Hyperkalemia shifts the membrane potential of the myocytes to a range between -65 and -40 mV. At this voltage, not all of the sodium channels are inactivated. Sodium influx by non-inactivated sodium channels [5,6] can lead to the activation of the sodium-hydrogen exchanger and intracellular acidosis [7,25,26]. Consequently, acidosis and ischemia lead to inhibition of the sodium/potassium-ATPase [26] and further increase the intracellular sodium. Sodium overload causes the sodium/calcium exchanger channel to act in reverse mode, increasing the calcium loading of the myocyte and leading to contracture and cell death [7].
One potential disadvantage of the LIRM solution compared to the HTK and G/A solutions is the inexistence of components that might supply the Krebs cycle, such as tryptophan in the HTK solution or aspartate and glutamate in the G/A solution. The absence such components might be responsible for the lower myocardial ATP content observed with the LIRM solution. The addition of some precursors of the Krebs cycle to the LIRM solution might improve the energy maintenance during cold storage, as assessed by the myocardial ATP content.
Study limitations
We did not evaluate hemodynamic data, such as left ventricle systolic and diastolic pressures, dP/dt maximun and minimum, and contractility indexes. Conclusions were limited to the period before reperfusion, but we were able to show a higher myocardial ATP content with the HTK solution, different caspase activities in all three groups, and higher effectiveness of the LIRM solution in achieving cardiac arrest.
CONCLUSIONS
The HTK solution was more effective in promoting higher levels of myocardial ATP content compared to the two other solutions. The LIRM solution was very effective in promoting cardiac arrest and reducing caspase 3 activity compared to the A/G solution. These preliminary data concerning the use of different pharmacological agents for cardiac arrest are promising. In the future, cardioplegic solutions containing Krebs cycle substrates, such as tryptophan and histidine, might be considered.
REFERENCES
1. Lewis FJ, Taufic M. Closure of atrial septal defects with the aid of hypothermia; experimental accomplishments and the report of one successful case. Surgery. 1953;33(1):52-9. [MedLine]
2. Melrose DG, Dreyer B, Bentall HH, Baker JB. Elective cardiac arrest. Lancet. 1955;269(6879):21-2. [MedLine]
3. Hearse DJ, Stewart DA, Braimbridge MV. Hypothermic arrest and potassium arrest: metabolic and myocardial protection during elective cardiac arrest. Circ Res. 1975;36(4):481-9. [MedLine]
4. Fallouh HB, Kentish JC, Chambers DJ. Targeting for cardioplegia: arresting agents and their safety. Curr Opin Pharmacol. 2009;9(2):220-6. [MedLine]
5. McAllister RE, Noble D, Tsien RW. Reconstruction of the electrical activity of cardiac Purkinje fibres. J Physiol. 1975;251(1):1-59. [MedLine]
6. Attwell D, Cohen I, Eisner D, Ohba M, Ojeda C. The steady state TTX-sensitive ("window") sodium current in cardiac Purkinje fibres. Pflugers Archi.1979;379(2):137-42.
7. Satoh H, Hayashi H, Katoh H, Terada H, Kobayashi A. Na+/H+ and Na+/Ca2+ exchange in regulation of [Na+]i and [Ca2+]i during metabolic inhibition. Am J Physiol. 1995;268(3 Pt 2):H1239-48. [MedLine]
8. Dunne MJ, Aspinall RJ, Petersen OH. The effects of cromakalim on ATP-sensitive potassium channels in insulin-secreting cells. Br J Pharmacol. 1990;99(1):169-75. [MedLine]
9. Rudd DM, Dobson GP. Eight hours of cold static storage with adenosine and lidocaine (Adenocaine) heart preservation solutions: toward therapeutic suspended animation. J Thorac Cardiovasc Surg. 2011;142(6):1552-61. [MedLine]
10. Stringham JC, Paulsen KL, Southard JH, Fields BL, Belzer FO. Improved myocardial ischemic tolerance by contractile inhibition with 2,3-butanedione monoxime. Ann Thorac Surg. 1992;54(5):852-9.
11. Peart JN, Headrick JP. Clinical cardioprotection and the value of conditioning responses. Am J Physiol Heart Circ Physiol. 2009;296(6):H1705-20. [MedLine]
12. Stringham JC, Paulsen KL, Southard JH, Mentzer RM Jr, Belzer FO. Forty-hour preservation of the rabbit heart: optimal osmolarity, [Mg2+], and pH of a modified UW solution. Ann Thorac Surg. 1994;58(1):7-13. [MedLine]
13. Wei L, Wu RB, Yang CM, Zheng SY, Yu XY. Cardioprotective effect of a hemoglobin-based oxygen carrier on cold ischemia/reperfusion injury. Cardiology. 2011;120(2):73-83. [MedLine]
14. Stockert JC, Blázquez-Castro A, Cañete M, Horobin RW, Villanueva A. MTT assay for cell viability: Intracellular localization of the formazan product is in lipid droplets. Acta Histochem. 2012;114(8):785-96. [MedLine]
15. Przygodzki T, Lapshina E, Zavodnik I, Sokal A, Bryszewska M. 2,3-Butanedione monoxime does not protect cardiomyocytes under oxidative stress. Cell Biochem Funct. 2006;24(5):413-8. [MedLine]
16. Drescher C, Diestel A, Wollersheim S, Berger F, Schmitt KR. How does hypothermia protect cardiomyocytes during cardioplegic ischemia? Eur J Cardiothorac Surg. 2011;40(2):352-9. [MedLine]
17. Viana FF, Shi WY, Hayward PA, Larobina ME, Liskaser F, Matalanis G. Custodiol versus blood cardioplegia in complex cardiac operations: An Australian experience. Eur J Cardiothorac Surg. 2013;43(3):526-31. [MedLine]
18. Chambers DJ, Fallouh HB. Cardioplegia and cardiac surgery: pharmacological arrest and cardioprotection during global ischemia and reperfusion. Pharmacol Ther. 2010;127(1):41-52. [MedLine]
19. Silveira Filho LM, Petrucci O Jr, Carmo MR, Oliveira PP, Vilarinho KA, Vieira RW, et al. Trimetazidine as cardioplegia addictive without pre-treatment does not improve myocardial protection: study in a swine working heart model. Rev Bras Cir Cardiovasc. 2008;23(2):224-34. [MedLine]
20. Lima-Oliveira APM, Azeredo-Oliveira MTV, Taboga SR, Godoy MF, Braile DM. Cardioplegia utilizando baixo volume de agentes cardioplégicos: Estudo morfológico em coração isolado de coelhos. Rev Bras Cir Cardiovasc. 2003;18:227-34.
21. Hachida M, Ookado A, Nonoyama M, Koyanagi H. Effect of HTK solution for myocardial preservation. J Cardiovasc Surg (Torino). 1996;37(3):269-74. [MedLine]
22. Radovits T, Lin LN, Zotkina J, Koch A, Rauen U, Köhler G, et al. Endothelial dysfunction after long-term cold storage in HTK organ preservation solutions: effects of iron chelators and N-alpha-acetyl-L-histidine. J Heart Lung Transplant. 2008;27(2):208-16. [MedLine]
23. Perrault LP, Menasché P. Preconditioning: can nature's shield be raised against surgical ischemic-reperfusion injury? Ann Thorac Surg. 1999;68(5):1988-94. [MedLine]
24. Oliveira MAB, Godoy MF, Braile DM, Lima-Oliveira APM. Solução cardioplégica polarizante: estado da arte. Rev Bras Cir Cardiovasc. 2005;20(1):69-74. View article
25. Pike MM, Luo CS, Clark MD, Kirk KA, Kitakaze M, Madden MC, et al. NMR measurements of Na+ and cellular energy in ischemic rat heart: role of Na(+)-H+ exchange. Am J Physiol. 1993;265(6 Pt 2):H2017-26. [MedLine]
26. Lahorra JA, Torchiana DF, Tolis G Jr, Bashour CA, Hahn C, Titus JS, et al. Rapid cooling contracture with cold cardioplegia. Ann Thorac Surg. 1997;63(5):1353-60. [MedLine]
This work was funded by Fundação de Amparo a Pesquisa do Estado de São Paulo (FAPESP) grant number 2012/09130-1
Author's roles & responsibilities
KR Implementation, writing and discussion
HRPC Implementation, writing and discussion
FL Execution discussion
AGT Writing and discussion
KASV Design, execution, writing and discussion
PPMO Discussion and manuscript review
LMSF Discussion and manuscript review
ESBOS Discussion and writing
OP Design, writing, analysis
Article receive on Tuesday, May 21, 2013
 All scientific articles published at www.bjcvs.org are licensed under a Creative Commons license
All scientific articles published at www.bjcvs.org are licensed under a Creative Commons license